What is Dry Needling?
Your Questions About This Pain Management Tool, Answered
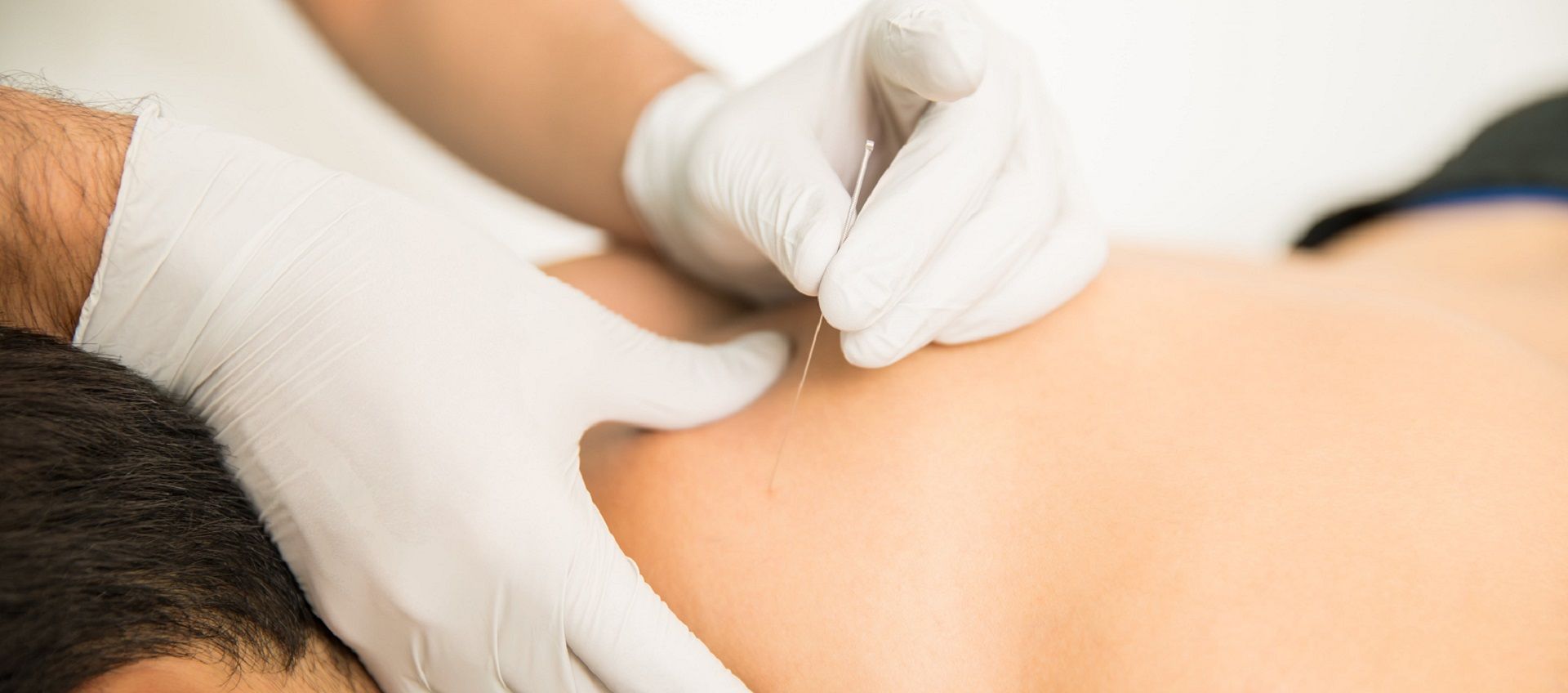
For patients struggling with certain types of muscular pain, a procedure called dry needling could be a useful part of their larger treatment plan for managing discomfort.
What is dry needling?
Dry needling is a technique in which a trained provider targets myofascial trigger points by carefully inserting fine needles, like the ones used in acupuncture, into the skin and layers underneath, sometimes including muscle. Myofascial trigger points are “hyperirritable spots in skeletal muscle,” according to an article on Physiopedia.com. The needles can be inserted on a superficial level (not penetrating as deep as the muscle layer) or a deep tissue level (penetrating the muscle), and it is called “dry” because nothing is being injected into the body from the needle, said Stephanie Barretto, physical therapist and manager of outpatient rehab services at PAM Health Rehabilitation Hospital of Corpus Christi. Dry needling is commonly used in conjunction with other pain management interventions such as exercise, stretching, and massage.
Explore Physical Therapy Offered by PAM Health
It’s also usually a supplement to a larger treatment plan, said Grant Henry, a physical therapist at PAM Health Rehabilitation Hospital of Clear Lake North.
“Like any type of passive intervention that we use, dry needling is typically an adjunct to a patient’s treatment plan. This is a tool we can use to help modulate a patient’s pain level or discomfort, allowing a window of time for the patient to participate in more active treatment approaches, like range-of-motion activities, functional strengthening, and activity tolerance, that can be more of a long-term solution,” Henry said.
The practice of dry needling in the United States dates back to the mid-1980s, with physiotherapists in other countries also beginning to utilize it around this time, as well. Over the past decade, the Federation of State Boards of Physical Therapy, the American Physical Therapy Association, and the American Academy of Orthopaedic Manual Physical Therapists all have expressed support for physical therapists’ use of the technique. Dry needling certification and continuing education courses have also increased in prevalence in recent years.
What and who is dry needling for?
Dry needling is an option for managing pain for “any type of musculoskeletal condition involving soft tissue restrictions or pain,” said Henry. For his patients, these conditions commonly include low back pain, neck pain, cervicogenic headache (headaches that originate from bone or tissue in the neck), TMJ (jaw-related) disorders, knee osteoarthritis, and shoulder pain. Other conditions for which dry needling might be used to relieve pain include whiplash-associated disorders, mechanical neck pain, tension-type headaches, migraines, rib syndromes, carpal tunnel syndrome, shoulder impingement syndrome, and tennis elbow.
“There is also some research supporting dry needling for reduction of spasticity in patients with stroke/upper motor neuron lesions, as well as with pelvic floor dysfunction,” Henry noted.
For patients experiencing these musculoskeletal and related conditions, trigger-point dry needling can offer benefits when it is determined they need further support beyond the more conventional pain management tools (e.g., exercise, massage, etc.), said John Henicke, a physical therapist at PAM Health Specialty and Rehabilitation Hospital of Luling. Therapists make sure to educate patients so they understand and feel comfortable with the procedure, Henicke added.
Henry agreed. “I would typically recommend dry needling in a few instances. For one, if a patient has had a previous good experience with either dry needling or acupuncture. Also, if we have exhausted other passive modalities (massage, manual therapy, electrical stimulation, etc.) without any success or improvement. And lastly, if we are able to easily identify a myofascial trigger point or hypertonicity at the area we are addressing,” Henry said.
How does dry needling work?
Dry needling works to improve pain symptoms in patients through different mechanisms that help increase the patient’s pain threshold and range of motion while also decreasing muscle tone and stiffness that can interfere with movement. These mechanisms are the “body’s natural pain relievers,” Barretto said, and include:
- Local twitch response, which is an uncontrollable reflex causing a localized contraction of the muscles undergoing dry needling. This reflex can help alleviate tension in the muscle fibers and stimulate mechanoreceptors, which play a role in a person’s sense of touch, to help decrease pain.
- Effects on blood flow: Sustained tension in myofascial trigger points can negatively impact blood and oxygen flow to organs and parts of the body. Dry needling can improve the blood and oxygen flow in muscles by dilating small blood vessels in the affected area.
- Neurophysiological effects: “Dry needling may trigger local and central nervous responses to promote hemostasis at the site of the trigger point which results in reduction in both central and peripheral sensitization to pain.” (Gattie, et al., 2017, pp. 133-149)
Once a needle is in place, the therapist may move it in and out a few times and/or stimulate the muscles. At the end of the treatment, the needles are removed. Patients may need more than one treatment session to optimize results, Barretto said.
Although dry needling and acupuncture use the same needles, the similarities end there regarding pain management. The two techniques find their origins in different medical traditions. Acupuncture originated in traditional Chinese medicine with the idea that the body and its organ systems intersect with meridians of energy, or “qi,” along the body and is used to treat a wider range of conditions, Henry explained.
On the other hand, dry needling traces its roots to Western medicine and evidence-based literature, Henry said. While acupuncture aims to address conditions on a more holistic, whole-body level, dry needling targets specific areas of the muscle where pain is occurring, i.e., trigger points or ligaments/tendons.
“There could be an overlap of the two interventions working together, due to the fact that the approaches to the treatments are very different (i.e, where the needles are being placed). A physical therapist and an acupuncturist could work well together to treat the entire system and simultaneously address any non-musculoskeletal components to the injury as well,” Henry said.
Does dry needling hurt?
The thought of having needles stuck in one’s skin may be unsettling to some, but if patients feel anything at all - sometimes they don’t, Henry said – it’s usually minimal, momentary pain. The sensation can also vary depending on the area of the body where it is done.
“There are some areas that tend to be more sensitive than others during application of the needle. The patient may feel a small prick or a quick sharp pain, but typically after the application of the needle to the desired tissue, the patient can’t really feel that the needle is even still inserted,” Henry said.
After the procedure, patients might be sore or develop slight bruising, Barretto said. Ice and/or heat can help with these after-effects.
What should patients consider before trying dry needling?
There are couple important considerations potential dry-needling patients should consider before undergoing the procedure.
At PAM Health outpatient centers that offer the service, including PAM Health Rehabilitation Clinic of Lockhart, TX, it is not available for children under the age of 16, Henicke said.
Patients in the following groups should also consult their healthcare providers before dry needling:
- Are pregnant.
- Are unable to understand the treatment.
- Have compromised immune systems.
- Have just had surgery.
- Are on blood thinners or have abnormal bleeding tendencies.
- Have certain conditions like vascular disease, epilepsy, diabetes, cancer, or HIV.
- Have metal allergies.
- Have lymphedema in the same area where the dry needling would be performed.
Dry needling also would not be a good fit for patients with a strong fear of needles. “We consider each patient’s tolerance towards the needles themselves. If a patient is overly fearful of getting shots or needles, this is not an intervention we will use,” Henry said.
Who performs dry needling?
According to Henicke, the following types of licensed professionals who have completed the required continuing education can perform dry needling:
- Physical therapists (PTs)
- Occupational therapists (OTs)
- Certified athletic trainers (ATCs)
- Doctors of Chiropractic (DCs)
- Physicians (MDs and DOs)
- Nurse practitioners (NPs)
- Physician assistants (PAs)
- Acupuncturists
Dry needling is usually done in an outpatient setting. However, under certain circumstances and with a licensed provider, it could be an option for inpatients, Henicke said, as long as it is discussed with and approved by the hospital’s leaders.
For qualified patients seeking to decrease pain and advance their journey toward recovery, dry needling may be an effective tool in the larger toolbox of therapies and techniques providers have at their fingertips.
Find a PAM Health Location Near You
Learn more about PAM Health’s outpatient locations, services offered, and specialty treatment areas here.
Bibliography:
“What Is Dry Needling?” Cleveland Clinic, Cleveland Clinic, https://my.clevelandclinic.org/health/treatments/16542-dry-needling.
"Dry needling." Physiopedia, 9 Nov 2022, 14:20 UTC. 10 Apr 2023, 20:33, https://www.physio-pedia.com/index.php?title=Dry_needling&oldid=320081.
Gattie E, Cleland JA, Snodgrass S. The effectiveness of trigger point dry needling for musculoskeletal conditions by physical therapists: a systematic review and meta-analysis. Journal of Orthopaedic & Sports Physical Therapy. 2017 Mar;47(3):133-49.
Iheanacho F, Vellipuram AR. Physiology, Mechanoreceptors. [Updated 2022 Sep 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK541068/
Unverzagt C, Berglund K, Thomas JJ. DRY NEEDLING FOR MYOFASCIAL TRIGGER POINT PAIN: A CLINICAL COMMENTARY. Int J Sports Phys Ther. 2015 Jun;10(3):402-18. PMID: 26075156; PMCID: PMC4458928.